Nutrition In Pregnancy
Eating for two, three or more!
The beginning of a beautiful new journey called life…
So you’re about to become a busy parent or you’re already a busy parent!! As your family begins to grow, so do the challenges of pulling off some excellent healthy meal options for everyone to enjoy!
Thames Valley Midwives wants to offer you the best recipes and ideas in order to create some awesome meals that are not only nutritionally valuable for your pregnancy, but will continue to assist in creating a healthy future for your children to follow in your footsteps.
We value teaching families to make better choices…and what better time to start!

What should you be eating when you are pregnant?

Being pregnant doesn’t exactly mean you NEED to eat for two or three or more. We recommend that you have a healthy variety of foods, low in sugar and relatively lower in carbohydrates. A diet high in sugars especially refined sugars, and carbohydrates can result in larger babies and contribute to the development of gestational diabetes or diabetes outside of pregnancy.
Gaining weight via the support of a nutritious diet is a natural part of pregnancy. Health weight gain supports your baby’s growth and development, and prepares you for breastfeeding.
Weight gain:
How much weight gain is recommended depends on a person’s weight before becoming pregnant. Most of the weight gain happens during the second and third trimesters.
To help you gain a healthy amount of weight, you need to consume a few more calories in the second and third trimesters. After baby, to support lacation, you must also consume a few more calories than you normally would. For most people during pregnancy, this means an extra two or three servings from any of the food groups daily, in addition to their recommended number of Food Guide Servings per day.


These extra Food Guide Servings can either be included as an additional snack, or can be added to your usual meals. Breastfeeding clients also need an extra two to three Food Guide Servings each day.
The Government of Canada has an interactive plate that follows Canada’s Food Guide.
The Eat Well Guide (UK) displays a plate of food that you may find visually helpful to balance your diet.
Snack ideas -

- Edamame.
- Marinated artichoke hearts.
- Dried unsweetened coconut.
- Pear slices with ricotta cheese.
- Spicy avocado.
- Flaxseed apple homemade muffins.
- Homemade protein bars.
- Keto banana bread – has no sugar, and can be made with coconut or almond flour.
- Smoothies – add fruit or veggies. Coconut milk or almond milk are good dairy-free alternatives.
- Guacamole or hummus with crackers, pita bread or cut up veggies.
- Nuts and seeds.
- Yoghurt and mixed berries.
- Apple slices with peanut butter.
- Celery sticks with cream cheese.
- Chia seed pudding – you can add cocoa powder for a little added sweetness without the sugar.
- Hard boiled eggs.
- Baby carrots with blue cheese dressing.
- Cheese and crackers.
- Whey protein shake.
- Dark chocolate pieces.
- Roasted chickpeas.
- Make your own popsicles in the summer with fruits, coconut, etc.
Tips:
Pinterest has lots of great recipes and snack ideas. Make sure you look for ideas that are lower in sugar. If your midwife is concerned about your baby getting too big, also make sure you support a diet with a lower amount of carbohydrates while boosting the amount of veggies and proteins you eat. Be aware that natural sugars are found in fruit – it still counts as sugar – so reduce your fruit intake too.
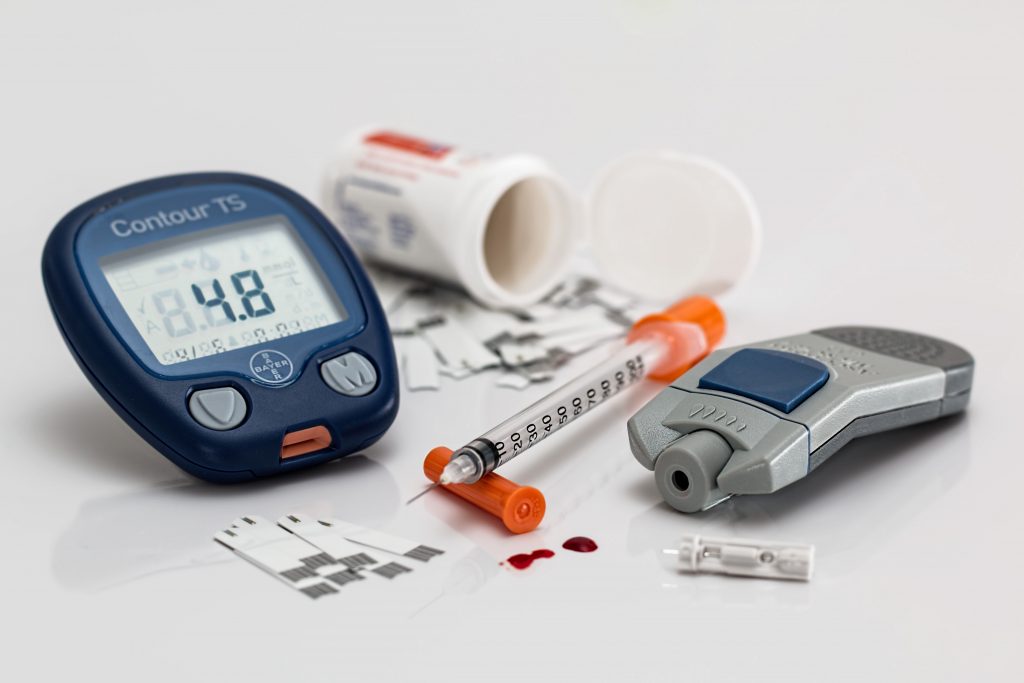
Gestational Diabetes
What is gestational diabetes (GDM)?
GDM occurs when the pancreas is unable to produce sufficient amounts of insulin to transport the glucose (sugar in your blood) to the cells in your body. In a normal person, blood sugars are regulated by insulin which is available to transport glucose into the cells.
Testing for GDM:
Your midwife will offer you routine gestational diabetes screening at around 28 weeks.
An early gestational diabetic screen is also offered to clients in early pregnancy if they have risk factors for developing gestational diabetes such as previous gestational diabetes, raised body mass index at or above 30 (BMI), age over 35 years old, strong family history of diabetes, polycystic ovaries, previous large baby, as well as a few other factors that your midwife may discuss with you.
What if I don't want the test?
If, after an informed choice discussion with your midwife, you decide not to have gestational diabetes screening, your midwife will monitor your pregnancy for indications of GDM and will discuss testing again at this point. You can then decide whether you want further testing or not.
GDM Diagnosis:
There are two different kinds of GDM:
- Insulin dependant
- Diet controlled
What next?
If you are diagnosed with GDM, we will refer you to the pregnancy endocrinology clinic, where you will meet with a specialized doctor to discuss the course of your pregnancy care. Often clients are given a diet to follow, with instructions of when to monitor their blood sugars, and a follow-up visit to discuss the findings. We also make referrals to an obstetrician for high risk pregnancy and a hospital dietician.
Will my baby be ok?
I'm on insulin, what now?
Midwives are experts in low risk pregnancies. When clients develop insulin-dependant GDM, their pregnancy becomes high risk, which falls outside the midwives scope of practice. We will at this point transfer care to an obstetrician. We will discuss whether you would prefer all of your care to be transferred or whether you would like the midwives to remain in a supportive capacity. Your midwife will discuss in detail what this might look like.

Click on the link below to see what a dietician can do for you.
References:
- Government of Canada – pregnancy weight gain calculator (2018)
- Government of Canada – How much food you need every day (2018)
- Government of Canada – Pregnancy and breastfeeding (2018)
- Government of Canada – Build a healthy meal (2016)
- Eat well guide U.K. (2016)
- Diabetes Canada – GDM clinical practice guidelines (2018)
