Your Care And What To Expect
Prenatal Care During Pregnancy

Regular prenatal care is essential for all pregnant families preparing for birth. This is a safeguard for your health and your baby’s health, as well as offering you the possibility to learn about the changes your body goes through as pregnancy advances.
Your Appointments:
Our care for you begins with a booking visit to discuss your plans, answer any questions and concerns, and review your health history. The first appointment is usually around an hour, over the phone in the first 12 weeks of pregnancy.
Over the course of your pregnancy, your midwives will discuss the choices you have for routine testing, ultrasounds, labour and birth, newborn care, choice of birthplace, changes your body incurs as your pregnancy advances, exercise, nutrition, and we counsel you about other wellbeing and emotional aspects you may be encountering during pregnancy. Some appointments will be in-person and some virtually, typically for around 30 minutes. Your midwife will check your blood pressure, your weight if you wish, general wellbeing, the position of your baby, monitor your baby’s growth, and check your baby’s heart rate. We may also perform an initial blood draw in order to monitor several blood levels that are important throughout pregnancy, if you haven’t already had these prior to seeing us.
If you are planning a surrogacy, we will discuss your plans regarding the intended parents throughout the pregnancy, also offering the intended parents the option to do virtual visits alone if they wish, to discuss their needs and concerns to prepare them on their journey to parenthood.
We schedule prenatal visits on a flexible schedule, based on individual client needs. This could mean that one client is seen more often than another. As you approach the end of your pregnancy, you will be seen on a more regular basis.
Your partner and children are welcome to attend appointments with you, and we request that we meet your partner or labour support person at least once. We also have at least one appointment with you alone.

If you are planning sibling participation at your birth, then it is important that your children get to know us and feel comfortable around us. If you find your little one(s) is/are a distraction for you, you may wish to arrange childcare for some visits.
If you have respiratory symptoms, you are ill or test positive for COVID-19, your midwife will schedule a phone appointment until you feel better.
During dangerous winter weather conditions, we will notify you of clinic cancellations. We almost always cancel clinics during times where schools and universities are cancelled due to dangerous driving conditions. Your safety and the safety of your baby are of utmost importance, as well as keeping your midwives safe too. You can also view our cancellation updates on our Front Page. Please check before leaving home that clinic is still running. If you ever feel you’re unable to safely come to clinic, we urge you to rebook for another day.
Home Birth Preparation:

Home birth became more popular than ever during the COVID-19 pandemic and still remains a safe and wonderful option for low risk clients. Our home birth rate sits around the 25% mark, with clients enjoying the benefits of remaining in the comfort of their own home to have their baby. If you are planning a home birth, we will do a prenatal visit with you at home when you are approximately 36 weeks pregnant, especially if this is your first home birth, so that we can easily locate your residence for the labour. We discuss our set up and your wishes/plans including planned waterbirth, and equipment such as oxygen, intravenous supplies, bloodwork supplies, newborn resuscitation equipment, and suction equipment.
This is also a good time to discuss other plans you may have like the inclusion of a birth photographer or a doula. We also like to discuss emergency procedures such as a transport to the hospital if necessary, during this appointment. You can read more about birthing at home in our home birth section.
Cancelling Appointments:
If you must cancel an appointment, we request that you advise us as soon as possible. If your primary midwife is unavailable due to attending a birth or vacation/off-call time, another midwife in the practice will see you. Due to rapid births or midwifery emergencies, we are often required to cancel your appointments with short notice. We will re-book you to the next available appointment time. During dangerous weather conditions, we will notify you of clinic cancellations. Our primary focus is on your safety and the safety of your baby.
Previous Practitioner:
If you have seen a family physician or another midwife for part of your prenatal care, it is very important we receive copies of your health records. This includes all blood work, urine tests, pap smear results, ultrasounds, etc, that were done. Obtaining these records ensures that we have a complete record of your care, and that you are not subjected to unnecessary blood draws or other tests. We will request that you sign a medical records release in order that we can obtain these from your previous care provider.
Our discrimination policy:
Most of our clients treat us as they would like us to treat them, but unfortunately, we occasionally experience anti-social behaviours such as discrimination against ethnicity and age, verbal abuse, harassment of midwives and staff of Thames Valley Midwives, and the use of discriminatory, threatening, abusive or menacing language. We ask that clients attending our practice, or working with our staff and/or practitioners (whether in-person or by telephone), behave in a manner, which respects the rights of others and the practice environment.
Thames Valley Midwives encourages mutual respect at all times and supports a harassment-free environment; as such discrimination, verbal abuse, and/or aggression directed to midwives or staff will not be tolerated. Any person acting in an unacceptable manner may be subject to early discharge from our care.
In keeping with the Ontario Human Rights code, we believe that every person has a right to be free from harassment and discrimination within our practice, and in any other environment in which we work with clients and their families.
What if your pregnancy becomes high risk?
Midwives provide total care to clients who experience healthy, normal pregnancies. If you develop obstetrical problems or develop a medical condition, you and your midwife will determine the appropriate source for your ongoing care. The College of Midwives standards for practice includes specific conditions of a client and newborn in which midwives must seek a medical referral. If it becomes necessary for your care to be transferred to an obstetrician, your midwife will discuss ongoing care arrangements. Depending on the complication, your midwife may be able to “share care” with an obstetrician, which means they will organize your prenatal care between the partnership and then decide who is most appropriate to deliver your baby. Your care may be completely transferred during your pregnancy, in which case your midwife can either transfer your care entirely or resume care after the baby is born. Where possible, your midwife may attend your delivery. If care is transferred during your labour, your midwife will often get you settled, then take a break to rest until your baby is ready to come, or will visit afterwards depending on your arrangement.
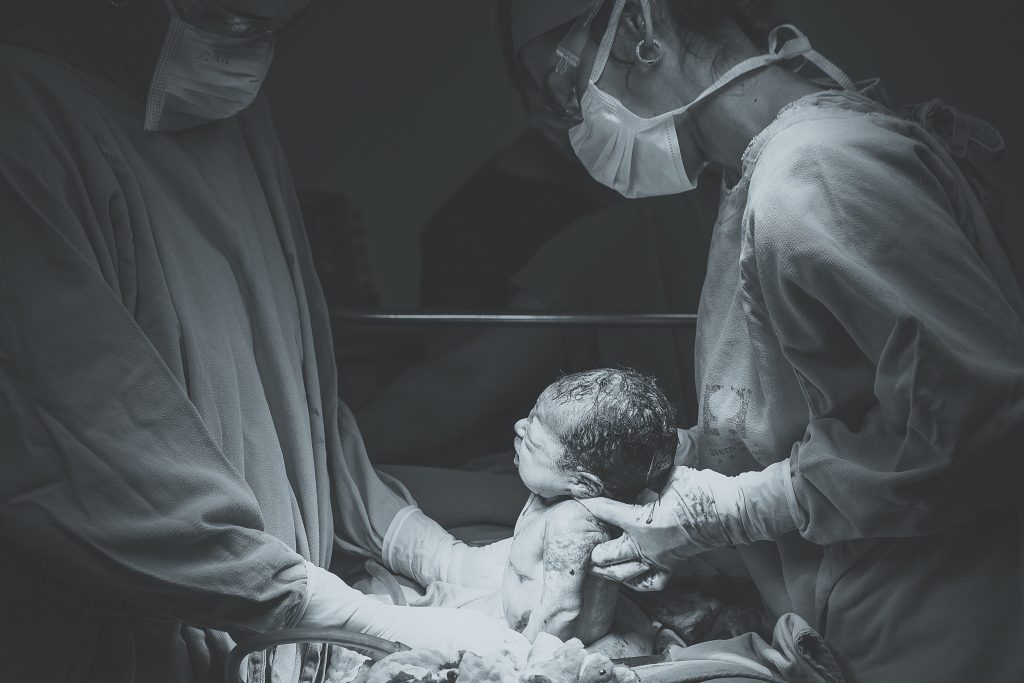
Prenatal Classes:
We strongly recommend that clients and their partners having a first baby attend prenatal classes. A brief list of classes can be found on our resources page, although other options are available. There are also refresher courses available to families who are not new to parenthood but want a “crash” course on labour, delivery and the newborn. There are many options for in-person and virtual available.
Labour And Birth

During the third trimester, your midwife will start to discuss your birth plans and when to call your midwife in greater detail. Our informed choice discussions throughout pregnancy will develop into plans for birth and prepare you for the “Big Day”! We attend births at London Health Sciences Centre Victoria Hospital in London, Woodstock Hospital in Woodstock, as well as in the Home.
In rare circumstances, when all the on-call midwives are attending births, or midwife resources are limited e.g. illness, bereavement or self-isolation for COVID-19, it may be necessary for clients planning a home birth to come to hospital to give birth. Similarly, clients may very occasionally be required to give birth at a hospital other than the one they had planned to use, either due to midwives already attending a birth at another facility or due to a lack of available labour/delivery beds at an individual facility. The majority of our hospital births take place at London Health Sciences Centre, therefore, clients planning births elsewhere may be required to give birth at London Health Sciences Centre.
During dangerous weather conditions, it may become necessary for your midwife to transfer your care to an obstetrician if planning a Woodstock Hospital delivery or if planning a home birth outside of London.
Clients under 37 weeks’ gestation are required to attend our level three hospital LHSC Victoria Hospital for any necessary hospital assessments. You should page your midwife before going to the hospital. Your midwife may instruct you on a necessary plan of care should you be unable to get to LHSC safely, which may include transferring to an obstetrician for the birth.
If you are planning to give birth at home, we will supply most of the necessary supplies (such as absorbent bed pads) and provide you with a list of household items which we expect you to have on hand for the birth. We will also discuss with you the indications and arrangements for transport to hospital. Please note that one requirement for a safe home birth is reasonably quick access to a hospital. We do require that homebirth clients who live rurally be within thirty minutes of a hospital, which offers obstetric services. In the event of inclement winter weather and poor road conditions, it may be necessary for rural clients at a distance to come to hospital for their birth.
If you are a client in our care, you can read more about your choices by clicking the link below.


When to page:
We wish to be contacted by you when you believe labour is established, and will review with you in the last few weeks of pregnancy what to look for.
Once your labour becomes active, your midwife will either meet you at the hospital or come to your home if planning a home delivery.
What will your midwife do?
During labour, your midwife will monitor labour contractions, blood pressure and other aspects of your well-being, fetal heart rate, check dilation of the cervix, assist with labour-coping techniques, conduct the delivery of the baby and placenta, suture the perineum (if required), examine the newborn infant and assess your condition after the birth.
One midwife is with you during active labour, and the second midwife is called when it is expected that the baby will soon be born.
Midwives provide skilled support during labour, and suggestions for coping with pain. However, we cannot replace the important support provided to you by your birth partner.

When to page:
We wish to be contacted by you when you believe labour is established, and will review with you in the last few weeks of pregnancy what to look for.
Once your labour becomes active, your midwife will either meet you at the hospital or come to your home if planning a home delivery.
What will your midwife do?
During labour, your midwife will monitor labour contractions, blood pressure and other aspects of your well-being, fetal heart rate, check dilation of the cervix, assist with labour-coping techniques, conduct the delivery of the baby and placenta, suture the perineum (if required), examine the newborn infant and assess your condition after the birth.
One midwife is with you during active labour, and the second midwife is called when it is expected that the baby will soon be born.
Midwives provide skilled support during labour, and suggestions for coping with pain. However, we cannot replace the important support provided to you by your partner, partners, close friends or other family members.
Postpartum Care

After your baby is born, we stay at your home or in the hospital with you for approximately two hours after the birth or until you are stable for us to leave. During this time we will assess your vital signs, bleeding, stitches if needed, assist with breastfeeding or formula feeding, check your baby thoroughly, whilst administering any medications to yourself or baby such as Vitamin K, assist you in the shower if you are mobile, provide you with some refreshments/snacks, clean up if you have had a home delivery, perform our record keeping, and provide information and guidance for your care during the early days after birth. If you have a caesarean section, your care will continue with the obstetrician until you are discharged home. Nursing staff will perform the above postpartum checks while you are in the recovery area and on the postpartum unit. Your midwife will perform the newborn check unless your baby is admitted to the neonatal intensive care unit (NICU).
Leaving or staying at the hospital:
If you give birth in hospital, you may have the option to go home directly from the labour and delivery room. If your birth has been uncomplicated, you and your baby are well, and there are no risk factors, a direct discharge is something you can discuss with your midwife after your birth. If you choose to have a direct discharge, the follow up care for you and your baby will be the same as if you had a home birth.
If you want or need to be admitted to the postpartum ward, you will be moved there a few hours after the birth. The minimum stay is six hours in this area if your birth was uncomplicated, and you and your baby are well. Rooms are semi-private with washrooms to share, or if you have coverage or wish to pay more, you can upgrade to a private room or suite for a fee. If you deliver at Woodstock General Hospital, you will either stay in the room you delivered in or be moved to a smaller postpartum room. These are generally all private rooms with your own washroom. While at the hospital, you will be taken care of by the nurses who will assist you with breastfeeding, caring for you and your baby’s physical needs. Should a complication arise, the nurse will contact your midwife for advice or orders.
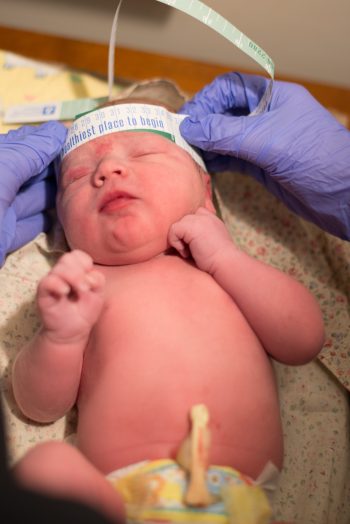

Home Visits:
The midwife visits you at home or at the hospital during the first week usually twice with a phone call in between visits, adjusting for clients who require further visits. We then see you at one of our clinics when your baby is two, and six weeks old with a four week phone call offered unless your baby needs an in person assessment for ongoing issues such as weight gain. Your midwife will do physical assessments for yourself and your baby as well as measure your baby’s weight, and offer tests such as the newborn screening blood test and congenital heart screening. Your midwife will also monitor your baby for jaundice and assist with breastfeeding. Since the midwife who is providing the home visits is also on-call for births, exact appointment times are not always possible and will need to be met with flexibility from the client. If you need to speak to someone about your home visits, please call the main office. Please do not page the on-call midwife about your home visits in case they are at a birth or sleeping. If it is more convenient for you to come to the clinic for your early postpartum visits, this can be arranged instead of home postpartum visits.
Discharging from the midwives:
At your six week discharge visit, we perform a pap exam if required, an assessment of your healing, discuss contraception among other topics, and carry out a full physical assessment on your baby. We send another letter to your family doctor and paediatrician regarding your health and the health of your baby so that they have all of the information required to follow up with your care.
During this six-week period, your midwife is available to you on a 24-hour on-call basis, as they are during pregnancy, for urgent concerns.
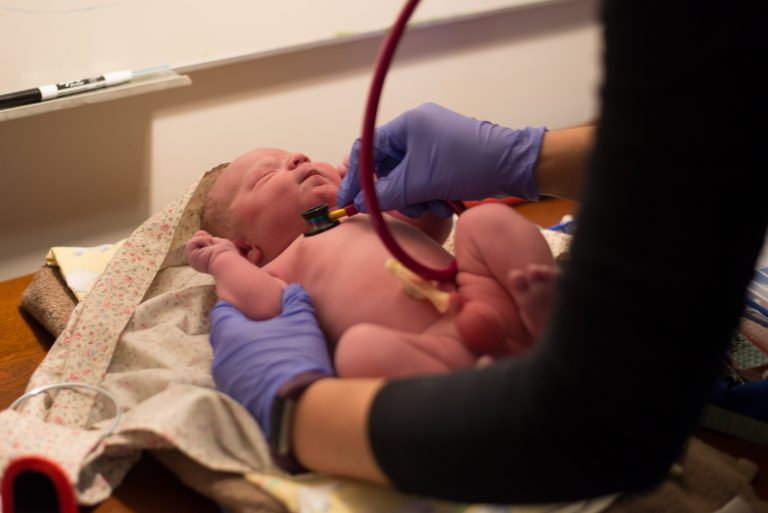
References:
- NICE antenatal care for uncomplicated pregnancy – U.K based prenatal care schedule and most current evidence based guidelines for uncomplicated pregnancy (updated 2018).
