Pregnancy
Physical changes during pregnancy
Nausea & Vomiting:
Feeling sick? You’re not alone! Many people experience nausea and vomiting during their pregnancy. That’s because changes in hormones can make you feel sick to your stomach. Certain smells and movements can make the nausea worse. The good news is that the nausea usually disappears after the first trimester, but unfortunately some people will have nausea and vomiting their entire pregnancy.
To help cope with nausea and vomiting, you can:
- avoid having an empty stomach, eat whatever food appeals to you in frequent small amounts, until you are feeling better,
- get out of bed slowly and eat soon afterward,
- drink fluids between meals, and not with meals,
- if you have been vomiting multiple times, try a rehydration tablet, packet or drink to assist with replenishing electrolytes and get lots of rest,
- take vitamin B6 supplements – 10-25mg 3 times per day,
- try acupuncture or acupressure wristbands,
- try ginger (ginger snaps or ginger cookies with natural ginger ingredients),
- choose cold foods (with less smell) or get someone else to do the cooking, if possible.

- get plenty of fresh air,
- try smelling fresh-cut lemons, mint or oranges – you can put them in an oil diffuser if you have one,
- try eating salty potato chips prior to a meal,
- brush your teeth after eating,
- avoid smoke, strong odours, alcohol and caffeine.
Constipation:
Many clients get constipated during pregnancy. It happens because food passes through your body more slowly when you are pregnant so you can absorb the extra nutrients you and your baby need. Eat foods high in fibre such as vegetables and fruit, whole grains, cooked or canned beans, peas and lentils. Drink more fluids, especially warm or hot fluids. Be physically active. There’s nothing like a good walk around the block to move things along! Warning! If you are pregnant, do not use a laxative to treat constipation without checking with your midwife first. Laxatives can trigger the onset of labour contractions.
Swelling (Oedema):
During pregnancy, you may notice some swelling in your feet and ankles in the third trimester. Pregnant people naturally retain more water in their bodies, so this is perfectly normal. Now is not the time to cut back on your fluid intake. Even when you feel bloated, you still need to keep drinking water and other fluids (like milk, fruit juice and soup) to stay healthy. To reduce swelling: put your feet up, avoid crossing your legs, wear loose clothing, and get plenty of rest and exercise.

Heartburn:
Heartburn is common during pregnancy. It is caused by the pressure of the growing baby and hormone changes during pregnancy that allow stomach acid to move up to your throat. The following suggestions might help:
- do not lie down after eating,
- when you do lie down, raise your head and shoulders,
- avoid fried or greasy foods,
- drink fluids between meals, not with meals,
- avoid coffee, colas, alcohol and smoking,
- eat slowly, take the time to chew well, eat small meals and snacks.
Some clients take an antacid medicine to help with heartburn. An antacid reduces the amount of acid in your stomach. Not all antacids are safe during pregnancy. Check with your midwife before you take one.
Braxton hicks contractions:
Braxton Hicks contractions are intermittent contractions of the uterus, which occur throughout pregnancy, but become more obvious as pregnancy progresses. Braxton Hicks contractions help the uterus prepare or practice for labour. These contractions are usually not painful, but painful Braxton Hicks contractions have been reported. In that case, it would clearly be a cause of abdominal pain during pregnancy.
Braxton Hicks contractions occur in every person that is pregnant, though not all may be aware of it. These contractions are usually felt within the last three months of pregnancy, though it could even be as early as the 16th week of pregnancy. Dehydration, tiredness or straining oneself could trigger these contractions. It is also very important to differentiate a Braxton Hicks contraction from false labour.
Signs and Symptoms of Braxton Hicks Contraction:
The following are signs and symptoms of Braxton Hicks:
- Braxton Hicks contractions are felt as a tightening on the abdomen. These could be rock solid. When felt with the hand, the hardness could be localized to a part of the uterus. After a few seconds to minutes, the contraction is followed by relaxation.
- These contractions could occur as early as the 16th week of pregnancy, but more often after the 20th week.
- They present as irregular contractions. This means that there may be no pattern to the manner of contractions. You could have one contraction in every five minutes or every hour. Each contraction could last for a few seconds to minutes. They can keep reoccurring continuously for weeks or months.
- The contractions may be significant enough to take your breath away. It could also be felt as a dull ache or even painful. Some expectant parents have been woken up from their sleep by these contractions.
- Braxton Hicks contractions are often felt earlier by expectant parents who have had previous babies and the pain may be more intense in these people.
- The pain does not worsen in intensity as labour progresses.

Should I call my midwife?
Braxton Hicks contractions are normal and do not require you to page your midwife. If they are strong and uncomfortable/painful, you can try to take a bath, relax and take Tylenol (acetaminophen) 1000mg orally, to relieve them until they subside. We also advise you to drink at least two large glasses of water, as dehydration will cause Braxton Hicks contractions to be more intense.
Difference between Braxton Hicks Contraction and True Labour:
It is important to differentiate Braxton Hicks contraction from true labour. Failure to do this may lead to premature and or birth of your baby in an unprepared and frightening environment. True labour is differentiated from Braxton Hicks contraction or false labour by the fact the following:
- Genuine labour contraction starts steadily and gets stronger over time.
- The pain starts from the back and spread over to the abdomen. It increases in intensity over time.
- It is not stopped by change in activity and does not slow down or get better after taking a bath.
- True labour contractions are painful, and this even become more painful with time.
- In early labour, the contractions could be as frequent as every 15 minutes, and each contraction lasting for 30 – 60 seconds.
- There may be a “show”: thick mucous mixed with blood from the cervix.
You can read about labour and when to call here.
Emotions during pregnancy
Although each pregnancy is unique, certain changes are common to all normal pregnancies. A basic understanding of physical and emotional changes of pregnancy helps a client to understand pregnancy and have a positive experience.
First trimester:
During the first trimester evidence of pregnancy is limited to missing a period and learning that the pregnancy test is positive. Some physical changes are apparent, such as fatigue, nausea, vomiting and breast tenderness. These symptoms are common and vary in intensity.
Emotions can be unstable, and feelings of depression are not uncommon, often for no apparent reason. It is commonly believed that the mood changes in pregnancy are caused by hormonal changes. The two main hormones that play a major role in pregnancy are estrogen and progesterone. A person’s emotions are characterized by mood swings, which can range from great joy to deep despair. Frequently a client will become tearful with little cause. When asked why they are crying, they may find it difficult or impossible to give a reason.
This situation can be very unsettling for the partner, causing the partner to feel confused and inadequate. Because the partner may feel unable to handle their tears, the partner often reacts by withdrawing and ignoring the problem. Since the pregnant person needs increased love and affection, they may perceive their partner as unloving and non-supportive. Once the couple understands that this behaviour is normal in pregnancy it becomes easier for them to deal with although it will be a source of stress to some extent throughout the pregnancy.
Initially, even if the pregnancy is planned, there is an element of surprise that conception has occurred. The client may experience some uncertainty about the pregnancy. Feelings that timing is wrong, that career or long-term goals may need to be delayed and/or financial stresses are common. Uncertain feelings may also be related to excitement about assuming the new role of mother, fears about carrying the pregnancy as well as labour and delivery. The pregnancy may not seem real until about the 12th week when the baby’s heartbeat can be heard with a Doppler.
Third trimester:
The third trimester combines a sense of pride with anxiety about what is to come in order for the baby to be born. During the final weeks of pregnancy, a person’s anxieties and fears may increase along with physical discomfort. You may experience sleeplessness because you are not able to find a comfortable position. Periodic contractions may cause discomfort as well as the position of the baby inside the uterus. You may feel very vulnerable to rejection, loss or insult at this time.

Second trimester:
The second trimester is somewhat tranquil. Morning sickness generally passes. The threat of miscarriage lessens. The highlight of the second trimester is feeling the baby move, called quickening, which generally occurs during the 20th week of pregnancy. Perception of fetal movement often leads to dramatic changes in a client. You will now perceive the baby as a real person and become excited about the pregnancy even if you were not prior to this time.
Clients sometimes have more energy and feel better during the second trimester, commonly known as the “glow of pregnancy”. Most clients begin wearing pregnancy specific clothing during this time. You may ask your friends and family about pregnancy, childbirth and may attend childbirth preparation classes.
You may feel unattractive and undesirable to your partner. Many of the nurturing and sexual needs of the pregnant client can be satisfied by cuddling, kissing and being held by your partner. The warm sensual feelings that are present during these times can be uplifting for you.
A client may be eager for the discomforts of pregnancy to end but could also be concerned about the reality of becoming a parent and the changes in spousal and family relationships, especially how a baby may affect other siblings. You may be concerned about the pain of labour, especially if you have had a previous unpleasant experience or have never experienced labour and have no idea what to expect. The health and well-being of the infant may preoccupy your thoughts during the last month of pregnancy.
The feelings and fears experienced during pregnancy are intense and varied. These feelings and concerns are a normal part of pregnancy. Each client comes to terms with the changes in their own way, with the support of their partner or family.
Recognizing preterm labour
What is preterm labour?
Preterm labour happens before 37 completed weeks of pregnancy and affect around 5-10% of pregnancies. Babies born prematurely may have many health problems.
Am I at risk for preterm labour?
You should let your midwife know if you have any of the following early identification risk factors including:
- Smoking, drug use, or alcohol
- Not eating properly
- Presence of infections (STD, bladder)
- Previous baby born prematurely
- Problem with pregnancy or medical illness
How will I know if it is preterm labour?
Your contractions will continue to become more painful, stronger and more intense despite trying to relax, take a bath, drinking lots of water and taking Tylenol 1000mg. Also if you experience your waters breaking (see labour) or bloody discharge from the vagina.
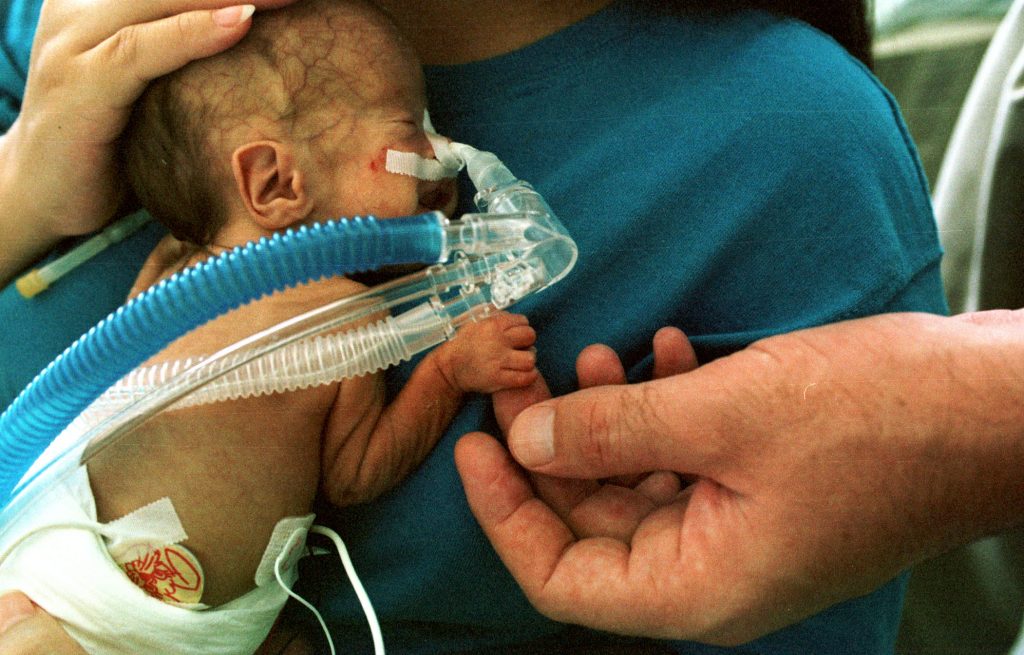
What can be done to prevent preterm birth?
Your midwife may:
- Put you on bed rest at home or in the hospital
- Tell you to have a good fluid intake
- Consult with an Obstetrician with regard to using medications to stop labour and to help mature the baby’s lungs.
Sleeping

First trimester:
Sleeping during pregnancy often gets worse during pregnancy and sleep disorders can present such as insomnia, sleep apnea and restless leg syndrome. Furthermore, physical symptoms of pregnancy like cramps and nausea, as well as the general discomfort of carrying a child to term, can greatly exacerbate sleep-related conditions.
During the first 12 weeks of your pregnancy, your body’s hormones will change significantly. Progesterone is a hormone that helps the non-pregnant person sleep. So when a higher level of progesterone is present in the body due to pregnancy, it can lead to excessive daytime sleepiness and disrupted overnight sleep. Sleep onset insomnia refers to difficulty falling asleep at normal bed times, while sleep maintenance insomnia is the difficulty remaining asleep. Increased progesterone levels can lead to either type of insomnia.
Even during the first trimester, you will need to urinate more frequently, because the blastocyst (little balls of cells which will become your baby) will apply pressure on your uterine wall, which is located near the bladder.
Strangely enough, bladder pressure has also been linked to lucid dreams (or vivid dreams) during pregnancy. Both of these factors may impact your ability to remain asleep through the night.
From 3-8 weeks of the first trimester, there are significant bodily changes for you and your baby including major organ growth for baby, and pelvic cramping with swelling of the breasts for you. These aches and pains can easily disrupt your sleep, as well. Additionally, you may experience excessive nausea, an affliction commonly called morning sickness.
By the ninth week, the embryo will have grown into a fetus, and the uterus will be the size of a large tomato. More cramping, swelling and discomfort typically occur until 12 weeks.
Here are a few tips for reducing physical pain and getting enough sleep during your first trimester:
- Nap frequently to counteract the effects of your rising progesterone levels during the first trimester. Experts suggest napping in the afternoon in order to maintain your nighttime sleep cycle; two catnaps, each lasting between 30 minutes and an hour, are considered more effective than one long nap.
- Exercising in the morning can also help you maintain healthy sleep cycle.
- Avoid consuming large amounts of fluid in the evening. This should reduce your urge to urinate in the middle of the night.
- If you experience morning sickness, try snacking on light, salty foods like popcorn or pretzels.
Second trimester:
During the second trimester, you will experience your baby beginning to move. Some people will experience this earlier than others, but generally around 18-22 weeks you should be able to feel some movement, even though it may not be every day yet. Your baby will be growing considerably during this trimester, and by 27 weeks will be around 10 inches on average and weigh more than a pound.
Sleep patterns are generally considered good during this trimester as your body will be acclimated to the rising progesterone levels, so daytime fatigue and sleep onset problems are usually less prominent, and morning sickness usually goes away. This is the best time to establish a healthy sleep schedule.
However, you may encounter some physical symptoms during the second trimester that negatively impact your sleep. Heartburn, for one, is quite common during this period, and lying down can often increase the discomfort of acid reflux.
Nocturnal leg cramps can also be an issue, particularly pains in the calf muscles usually at night. Although these will probably become more pronounced during the third trimester, cramping often begins during the second. If you’re prone to lucid dreams, then you can expect these to intensify during the second trimester, as well.
Here are some tips to help with sleep hygiene:
- Avoid eating and drinking certain things to ensure these second-trimester symptoms won’t be too severe. Spicy or fried food can lead to heartburn flare-ups, while soft drinks and other carbonated beverages can worsen the effects of leg cramping.
- Try to stand or sit upright for at least four hours after eating in order to ease the digestive process and mitigate your heartburn.
- If you experience a leg cramp in bed, try flexing your leg and/or foot muscles to relieve the temporary pain.
- Reduce screen time (T.V, social media apps, phone use) at least an hour before bed and do something relaxing like listen to relaxing music, meditate, read a book.
Third trimester:
At 28 weeks, the third trimester begins and your baby will grow rapidly. This means you will develop more aches and pains causing severe lower back pain as you gain excess weight, more intense leg cramping, frequent urination will return as the baby settles in your pelvis, and 20% will suffer with restless leg syndrome (characterized by painful tingling or itching sensations).
All of these factors can seriously disrupt sleep routines; the vast majority of pregnant people wake up between three and six times each night during their third trimesters.
Here are some tips for sleeping:
- Reduce fluid intake in the late afternoon or evening to prevent overnight runs to the washroom.
- Ensure your bladder is completely empty before going to bed. Leaning completely forward while peeing can help.
- Avoid eating anything that irritates your digestive system, and consume plenty of iron-rich foods to help with restless leg syndrome and excessive leg cramping.

- Stretching and light exercise before bed can help you fall asleep more quickly.
- Sleep on either side to relieve pressure on your lower back. This will also boost your circulation.
- Place pillows between your knees, behind your back and beneath the underside of your stomach for more comfort.
Encouraging labour to start:
It is considered normal for a pregnancy to last up to 42 weeks. Only around 5% of babies are born on their due date! Most client carry their babies for longer than the expected 40 weeks. At this stage in your pregnancy, you may feel ready to stop being pregnant and you may find these last day of waiting to meet your baby physically and mentally challenging.
Although it is unlikely that the methods described below will give you an immediate result, any combination may be helpful in preparing your body and mind for labour. They are not meant to be “solutions” for the post term pregnancy, in fact, treating them as such is likely to reduce their effectiveness! The further into your pregnancy you are, the more likely your body will respond. Patience is an important element of allowing your body to do what it needs to do – especially when preparing for labour.
It is important NOT to try these methods until you are term and your midwife has said it is safe to do so.
The following methods may be used for encouraging labour:
- Red Raspberry Leaf Tea – the most commonly used herbal tonic for strengthening the uterus. It should be used regularly (at least daily, after 37 weeks) for the best effect. It does not make contractions stronger but enables the uterus to contract more effectively, thereby shortening the length of labour.
- Exercise – staying active helps the baby to engage deep into the pelvis where contact between the baby’s head (or forewaters) and the cervix help to stimulate contractions. Going for walks can also be a good stress reliever. Gentle bouncing and rocking while seated on a birthing (exercise) ball is also a great way to open the pelvis and encourage the baby’s head to descend. Yoga and squatting positions can also be useful for engaging your baby’s head and relieving stress.
- Evening Primrose Oil – is an agent that encourages ripening of the cervix by imitating the function of prostaglandin (a hormone) which your body naturally produces to prepare the cervix for labour. The usual dose is 2-3 capsules of 500mg daily. Insert 2 capsules high into the vagina before bed time, and take 1 capsule orally with. meal in the day time. You may want to wear a panty liner as it can be messy when you first get up in the morning.
- Homeopathic Remedies – it is best to discuss the use of homeopathic remedies with a homeopath as they can give you specific instructions tailored to your circumstances. Most homeopaths carry a range of natural remedies which have different effects at different stages of labour and pre-labour. Commonly used remedies include caulophyllum, cimifuga and pulsatilla. Some remedies are combined into a tincture/pill form known as “easy birth”.
- Relaxation – anxiety, fear and frustration play a major role in inhibiting labour. These feelings produce stress hormones in the body that work against the hormones which are trying to activate labour. Try to discuss your concerns with your midwife, and involve your support person (people) if possible. Aromatherapy is commonly used for relaxation and has a well documented, positive effect on getting labour started. It is best to seek advice from an aromatherapist. Commonly used essential oils for getting labour started include clary sage, lavender, rose, peppermint and frankincense.

- Sex – semen is rich in prostaglandins which help to ripen the cervix. Also, by orgasming you can produce oxytocin – the hormone needed to start labour! As the vagina has an increased supply of blood vessels during pregnancy, it is not unusual to have a small amount of fresh bleeding after sexual intercourse. This bleeding is from the vagina, not the uterus and therefore is not dangerous to the baby. It usually settles soon after the event. If you are worried about the amount of bleeding, contact your midwife.
- Hand expressing and Nipple Stimulation – Gentle massaging of the nipples helps to increase oxytocin levels in the body. It is essential that you do this in a relaxed manner and environment so that the stress hormones that inhibit labour are not initiated. Using your index finger and thumb and placing them opposite each other on the bottom and top edge of the areola (the darkened area around your nipple), bring your thumb and finger together by making a “V” shape into the tissue behind your nipple. You may see drops of colostrum forming on the edge of the nipple. You can do this for 10-15 minutes on each breast several times per day. Alternatively, you can use an electric pump 10-15 minutes/day to help increase oxytocin levels.
- Stretch and Sweep – this is also known as a membrane sweep. It is a procedure your midwife will offer you around 40 weeks into your pregnancy. It involves a vaginal examination in which the midwife will try to put her finger through the opening of the cervix to separate the membrane from the bottom of the uterine wall. This encourages the body to produce prostaglandins which will help soften your cervix. Repeating this procedure can be a useful method of encouraging the body to go into labour.
- Castor Oil – encourages uterine contractions as a result of gastric activity. Please discuss the use of castor oil with your midwife before you try this option.
Labour requires lots of energy, therefore it is important that you feel physically and mentally strong at the onset. Try to get plenty of rest, plenty of fluids and eat good food so that your energy levels are well stocked before you go into labour.
Remember…
Don’t be discouraged if after you have tried all the above and you have not gone into labour. Your body is not quite ready. Stay positive and calm, your baby will soon be here!
